Press release —
Discovery Health boosts access to cutting-edge digital healthcare innovation in 2021
Johannesburg – 30 September 2020
Today, Discovery Health announced the latest in business innovations and product enhancements designed around quality care for Discovery Health Medical Scheme (DHMS) members.
Extensive investment in a patient-centric ecosystem
“The COVID-19 pandemic has led the headlines in defining the challenge facing our healthcare systems this year,” says Dr Noach. “We have closely followed and analysed the local and global trajectory of the pandemic and have identified a tipping point for healthcare consumers to access healthcare differently, revealing opportunities for greater efficiencies in the future.”
Four key trends have emerged as currently dominant in shaping the healthcare industry:
- The COVID-19 pandemic has disrupted typical healthcare patterns and created discontinuity in the supply and demand of healthcare services.
- The global focus on patient-centric care is driving demand for improved quality of care and healthcare outcomes.
- Providers and consumers are increasingly leveraging digital healthcare services and big data capabilities to deliver better healthcare outcomes, more efficiently.
- In the time of great economic uncertainty there is a need to focus on broadening the affordability and accessibility of healthcare to as many people as possible.
“These are the tenets that have underpinned Discovery Health’s response to the pandemic and current healthcare landscape as a whole. COVID-19 has demonstrated the need for companies to innovate quickly in a short space of time, with the demand for digital healthcare services in particular, rising significantly. We have maintained a rapid pace of innovation across the scheme’s value chain, and regularly lead the market with new technologies, tools and benefits to offer better value, greater quality and an enhanced member experience.”
Introducing access to cutting-edge, digitally Connected Care across the continuum
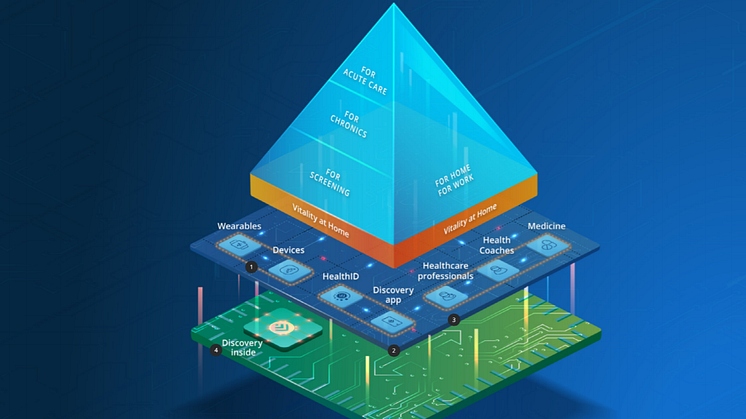
Discovery Health has invested extensively in a digital healthcare ecosystem to enhance the quality and experience of healthcare for members of DHMS. This investment includes the adoption and funding of digital healthcare technology, digital tools for members and doctors, integration with health monitoring devices and sophisticated data analytics.
For 2021 Discovery Health has consolidated and enhanced the digital healthcare experience through Discovery Connected Care. Discovery Health has integrated Connected Care with a range of industry leading healthcare devices for remote diagnostic and monitoring. DHMS members gain enhanced benefits for home-based healthcare services enabled by Connected Care, including the funding of integrated healthcare devices.
“We are excited about this cutting-edge digital platform which offers members a consolidated digital healthcare experience across the care continuum. Connected Care enables a range of appropriate home-based healthcare services for all levels of care, funded by Discovery Health Medical Scheme,” explains Dr Noach.
Connected Care for members, in the comfort of home
The increased adoption of digital healthcare, accelerated by COVID-19, has highlighted the patient’s home as an important and relevant setting for healthcare.
Connected Care for members at home revamps the virtual consultation experience by bringing it closer to a face-to-face doctor visit. It achieves this by linking the latest in diagnostic point-of-care technology, e-scripting and medicine delivery, all accessible from the comfort of the member’s home.
“Discovery has long offered platforms for virtual consultations with healthcare providers to our medical scheme members. Now, we are proud to announce that, for the first time in South Africa, Discovery Health is giving access to a remotely guided doctor visit by connecting the internationally acclaimed TytoHome device to the member’s virtual consultation. This sophisticated clinical device enables remotely-guided, clinical-grade virtual consultations with a GP anywhere, anytime,” explains Dr Noach. “The TytoCare device sends the doctor a live feed clinical-grade images and sounds during a virtual consultation, so that the GP can accurately diagnose and prescribe treatment for common conditions, no matter where the patient is located.”
The kit includes an examination camera, thermometer, otoscope and stethoscope and allows a user to capture and share not only ear, throat and skin images but also lung and heart auscultations (sounds typically heard with a stethoscope) and share these easily with a doctor in the TytoCare Doctor Network.
“Members are able to access trusted medical advice and an accurate clinical diagnosis from a nationwide network of experienced healthcare providers who are trained in and equipped to facilitate Tyto-enabled virtual consults,” adds Dr Noach. Members also received a post-consultation dashboard including their updated Electronic Health Record, e-script, treatment plan, sick note and relevant referral appointments.
Cutting-edge technology optimises care for chronic conditions
Connected Care for chronic conditionsprovides members living with chronic conditionswith end-to-end digital chronic delivery and management through access to personalised coaching, consultations and remote monitoring devices to better manage and track chronic conditions at home.
“The advanced, integrated reporting process provides automatic trigger alerts to a member’s treating doctor,” explains Dr Noach.
Discovery Health Medical Scheme offers members a number of condition-specific care programmes managed through the Premier Plus GP Network and providing benefits, care pathways and digital tools to achieve well-coordinated care for members and to allow for optimal management of their condition. In 2021, the Diabetes Care, Cardiac Care and Mental Health programmes will be enhanced through the Connected Care Platform as members will access digital condition-specific clinical content, integration with remote health monitoring devices appropriate for their condition and personalised health coaching.
Optimising acute care in the comfort of home
Connected Care for acute care at home provides qualifying members with clinically appropriate and patient-centric hospital-level care in their homes, as a substitute for acute hospital care.
“Globally, there is increasing evidence justifying treatment of some acute medical illness at home,” explains Dr Noach. “The convergence of our clinical and data insights has allowed for the identification of those cases that lend themselves to high-quality home-based acute care. This care applies in the case of early discharge from hospital, where there is a risk of readmission to hospital, in lieu of hospitalisation, or where acute care is required as end-of-life palliative care.”
“Generally speaking, home-based care enhances a member’s recovery experience, allows for highly-personal quality care and enhances patient safety. This form of care mitigates against underlying health risk and provides sufficient support and care to enable optimal recovery and improved outcomes.”
“Earlier this year DHMS led the market with the WHO Global Outbreak benefit, to provide testing and treatment for its members diagnosed with COVID-19. Notably, through the convergence of advanced data capabilities, the funding of pulse oximeters for high risk members diagnosed with COVID-19 has resulted in excellent preventative care, significantly improving health outcomes at an astounding 38% improvement in mortality.”
Ongoing improvement to mental wellbeing support systems
Every year the burden of mental illness on individuals and healthcare systems grows, placing a significant emotional and economic burden on society. World Health Organization (WHO) data show that 1 in 4 people will be affected by a mental health disorder at some point in their lives, placing mental disorders amongst the leading causes of ill-health and disability worldwide. The WHO also estimates that the cost to the global economy of mental health problems will exceed $16 trillion by 2030. Many people with mental health conditions often remain undiagnosed, with up to 84% of adults never receiving treatment.
“In 2020, this trend has been exacerbated by the devastating effects of the COVID-19 pandemic on individuals and societies,” says Dr Noach. “Our efforts to enhance access to digitally enabled, personalised, quality care for scheme members would not be complete without a focus on mental healthcare.”
Discovery Health offers a holistic approach to the management of mental wellbeing. DHMS members have access to clinically appropriate care management and intervention programmes for all levels of mental health, supported by networks of healthcare professionals, hospitals and psychiatric facilities.
- From 2021, Discovery Health’s existing Mental Health programme has been enhanced to offer:
- A Relapse Prevention Programme which will provide clinical support and benefits for members that are at risk of a recurrence of a major depressive episode (10-13% of DHMS members who are admitted for Major Depression are likely to have a second admission within 30-90 days of discharge).
- Enhanced out-patient care benefits to manage the transition from hospital to out-of-hospital care for major depression, including additional mental healthcare services for an extended period (40-50% of DHMS members who are admitted for a major depressive episode have a follow up consult with a healthcare provider within 30 days of their admission).
- Free access to Vitality Active Rewards Personal Health Goals for DHMS members at risk of or diagnosed with major depression. The Personal Health Goals will allow members to track their own health progress and be rewarded for completing their mental health checks and tracking their mental wellbeing.
Furthermore, Vitality and Healthy Company clients have access to world-leading incentive-based programmes to measure and manage the risks associated with mental wellbeing.
Launch of Shari’ah compliant plan options
In conjunction with leading Islamic scholars, Discovery Health Medical Scheme has created the Shari’ah Compliant Agreement.
From 2021, members of Discovery Health Medical Scheme will be able to elect to have their contributions and claims on any DHMS plan managed and invested in accordance with Shari’ah principles and managed through the Shari’ah-Compliant Arrangement. An Independent Shari’ah Advisory Committee has also been established by Discovery Health to secure the upfront ongoing compliance of all products and services marketed as Shari’ah compliant.
“The DHMS Shari’ah Compliant Agreement will be subject to regular reviews and annual compliance audits, assuring members of the Muslim community of compliance with Shari’ah principles,” explains Dr Noach.
Specific focus on 2021 Discovery Health Medical Scheme Benefit updates
1. Launch of cover for infertility treatment: “The inability to fall pregnant is a stressful problem affecting over 100 million couples worldwide,” explains Dr Noach. “With medical advances in the infertility treatment field, the majority of fertility cases are treatable with therapies such as drug treatment, surgical repair and assisted reproductive techniques such as Intra-Uterine Insemination (IUI) and In-vitro fertilisation (IVF).”
“Fertility treatment is highly individualised. Treatment plans vary considerably as every patient case is unique. With an average cost of between R65 000 – R85 000 for a single IVF cycle, the cost of infertility can be prohibitive.
To support members affected by infertility, in 2021 DHMS is introducing the Infertility and Assisted Reproductive Therapy benefit, to provide cover for Assisted Reproductive Technologies, such as:
- In-vitro fertilisation (IVF)
- Intra-uterine insemination (IUI)
- Frozen embryo transfer (FET)
- Intra-cytoplasmic sperm injection (ICSI)
Female members aged 25-42 years old, on Executive and Comprehensive Plans (who have been members for at least two years) will have access to the benefit, with cover for up to two cycles of ART (if they meet scheme benefit and clinical entry criteria).
2. Diabetes Care Programme enhances access to holistic care: It’s relevant to consider one of Discovery Health’s programmes condition-specific care programmes, Diabetes Care. This is a comprehensive programme for the effective management of diabetes. This programme has been enhanced for 2021 through the introduction of Connected Care for chronic conditions.
Members registered for the Diabetes Care Programme benefit from risk-funded benefits for consultations with a dietitian and biokineticist, and access to a nurse-led diabetic education programme. The Scheme also created the Premier Plus GP Network to support the Diabetes Care Programme (The network is currently the Designated Service Provider (DSP) for members with diabetes on the Priority, Saver, Core, Smart and KeyCare plans).
From 2021, the following changes will be introduced to the Diabetes Care programme:
a. The Premier Plus GP network will become the DSP for members with diabetes on the Comprehensive plans. This is supported by extensive coverage offered by the Premier Plus GP network and the clinical outcomes achieved by the Diabetes Care programme.
b. Members are enrolled onto the programme by their chosen Premier Plus GP who becomes the member’s DSP for the ongoing management of diabetes as well as cardiovascular conditions. Alternatively, members may nominate a Premier Plus GP as their DSP. This ensures that the member’s care is coordinated by a single doctor, which has been shown to improve clinical outcomes for members with multiple chronic conditions.
3. Expansion of Hospital Networks: To ensure continued optimisation of the Delta, Smart and KeyCare hospital networks, in 2021 new hospitals will be added and some existing hospitals will be replaced with region specific substitutions.
The DHMS hospital network lists will be published by the end of October 2020.
4. Formulary changes affecting chronic Drug Amounts: From 1 January 2021, certain formulary changes and Chronic Drug Amount updates will be applied. “We have been communicating these changes to impacted members. These members will have until the end of 2020 to make changes to their treatment and to avoid or reduce co-payments,” explains Dr Noach.
5. Limits, co-payments and deductibles: For 2021, co-payments and deductibles are increased by 3.5% to 4%. And, benefit limits are increased by 3%, with the exception of the following, for which there is no increase in 2021 – Oncology Threshold, Specialised Medicine and Technology Benefit, International Travel Benefit, Overseas Treatment Benefit, KeyCare mobility Benefit.
6. Co-payments for endoscopic procedures: Currently the scheme applies a co-payment of between R3750 and R4550 to in-patient gastrointestinal scopes on all of its plans except the KeyCare plans (where endoscopic procedures are only covered as PMBs). No co-payment applies to gastroscopies, colonoscopies, proctoscopies and sigmoidoscopies performed in the doctor’s rooms and for confirmed PMB cases. In 2021, to ensure that scopes are performed in the appropriate setting and to promote improvement in quality outcomes the following updates to the co-payment structure apply:
- DHMS will continue to apply no co-payment where scopes are performed in doctor’s rooms and/or endoscopic suites.
- A reduced co-payment of R3650 on all plans (except KeyCare) for scopes performed in day clinics.
- A co-payment of between R5300 and R6250 (depending on the chosen plan) will be applied for scopes performed in acute hospitals.
- Where an out-of-network deductible also applies for scopes performed outside of the Day Surgery Network, the higher of the benefit deductible or the out-of-network deductible applies.
- Where both a colonoscopy and gastroscopy are performed in the same admission, the higher co-payment applies.
An ongoing commitment to affordable, patient-centric healthcare
“At the end of the day, all of these innovations and developments are a manifestation of our drive to enhance access to affordable, efficient, on-demand, cutting edge healthcare across the continuum,” says Dr Noach.
“The integration of digital technologies is integral to creating platforms and support systems that allow us to focus on patient-centric, ever more personalised pathways. Most importantly we are committed to maintaining a focus affordability and sustainability into 2021 and beyond.”
- Read the full detail around all of these innovations and enhancements in the September 2020 Health Discoverer.
REFERENCES
WHO: Mental disorders affect one in four people
ENDS
For more information, contact
Nthabiseng Chapeshamano (084 037 1951)
Senior Reputation Manager
nthabisengc@discovery.co.za / media_relations_team@discovery.co.za
Topics
Discovery information
About Discovery
Discovery Limited is a South African-founded financial services organisation that operates in the healthcare, life assurance, short-term insurance, savings and investment and wellness markets. Since inception in 1992, Discovery has been guided by a clear core purpose – to make people healthier and to enhance and protect their lives. This has manifested in its globally recognised Vitality Shared-Value insurance model, active in 24 markets with over 20 million members. The model is exported and scaled through the Global Vitality Network, an alliance of some of the largest insurers across key markets including AIA (Asia), Ping An (China), Generali (Europe), Sumitomo (Japan), John Hancock (US), Manulife (Canada) and Vitality Life & Health (UK, wholly owned). Discovery trades on the Johannesburg Securities Exchange as DSY.
Follow us on Twitter @Discovery_SA